Important general principles to consider before proceeding with a hair transplant
12th April 2022
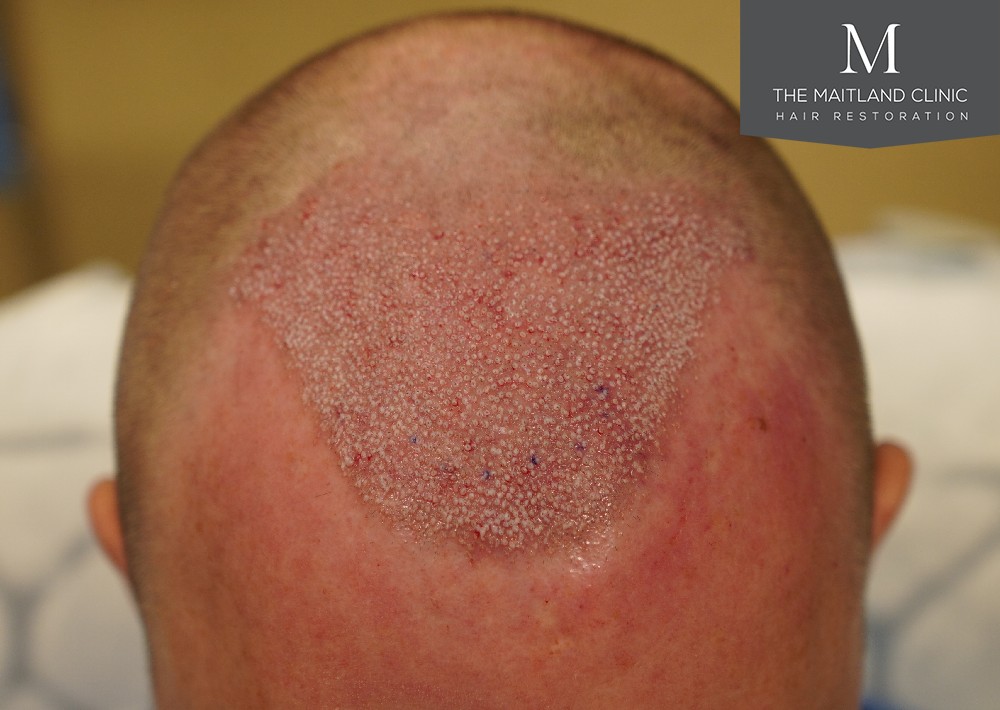
Limitations of hair transplantation
It is important to appreciate that hair loss is progressive. Therefore, your decisions need to take into consideration future hair loss and ensure that a new hairline will suit you now but, equally importantly, in later life.
There is only a limited supply of hairs/grafts at the back of your head available for transplanting (each graft that is taken for transplanting does NOT grow back and the supply will eventually run out). Dr Ball will advise how to make the best use of this finite number of hairs in order to achieve maximal impact.
It is not possible to recreate the actual density of hair you once had (the top of your head once possessed around 60,000 hairs and an average hair transplant procedure moves 1000-3000 follicular unit grafts). However, a hair transplant can create the impression of a dense coverage of hair. This is best done by placing the transplanted hair in a focused area to obtain maximal visual impact, rather than spreading that same number of grafts over a large area, with an inevitable thinner appearance. Despite this principle, some patients opt for a thinner “coverage” over a large area rather than more density in a restricted area.
Many patients opt for more than one hair transplant procedure in order to address a different area of hair loss (which had not initially been addressed or has developed due to ongoing hair loss) or to add even more density to a previously transplanted area. This would usually be performed no sooner than 1 year after the previous hair transplant so that the donor area has fully healed and the new hair growth has revealed itself.
Hair loss is usually an ongoing process, making it important to consider non-surgical treatments to help retain, and even thicken, your existing hair. These include Propecia tablets (finasteride), Regaine foam (minoxidil), low-level laser therapy (LLLT), platelet-rich plasma injections (PRP) or vitamin and mineral supplements. Dr Ball can advise you on these options.
It is possible that you will not have enough donor hair to cover all your areas of hair loss during your lifetime. Hair loss medication helps to improve the chances of your donor supply being sufficient to address your areas of hair loss.
Hair loss medication can be effective at slowing the rate of hair loss, stabilising hair loss or even thickening your hair. However, the benefits of medication tend to reduce over time and hair loss is likely to recur. A hair transplant plan needs to assume that hair loss will ultimately progress and therefore transplanted hair should only be placed in areas that will continue to look natural in the event of your native hair continuing to thin.
Lowering your hairline will use up many more grafts, making them unavailable to address areas of hair loss elsewhere (and, if lowered excessively, may look unnatural in later life).
It is uncommon for us to be able to transplant hair into the crown because continued hair loss can create an unnatural-looking island of grafted hair. The limited remaining supply of donor hair is likely to be required to treat continued thinning in the frontal half of the scalp, which is usually considered to be a higher priority area.
Scarring
Scar appearance and width will vary greatly from patient to patient. We use the very latest techniques to give every patient the best chance of scarring.
Follicular unit excision (FUE) leaves dot scars in the donor area where the grafts have been removed. These can appear as white spots, usually measuring 0.5-2 mm in diameter. These dot scars are usually well concealed by hair worn grade 1 or longer in the donor area (usually back and sides of the head). Patients wishing to wear their hair shorter than grade 1 should be aware that the white dots may be visible.
Follicular unit transplantation (FUT)/strip surgery leaves a linear donor scar at the back/sides of the head. The length of the donor scar will vary depending on the number of grafts required for transplantation, the density of the donor hair (how many hair follicles per square cm) and the laxity of the scalp skin. FUT scars tend to vary between 10 – 30 cm in length, depending on the size of the surgery. A 10 cm scar would usually be located at the back of the head, whereas a 30 cm scar would extend around the back of the head to above (and sometimes in front of) the ears.
We aim to provide our FUT/Strip patients with the best chance of healing with a thin, subtle scar. However, scar appearance is very much influenced by your own skin characteristics and healing ability and this can not always be predicted. Despite optimal surgical technique, some patients may have a natural tendency to form stretched or wide scars. An average FUT scar is likely to be between 1 and 5 mm wide. The width of a scar may vary along its length, with the mastoid area (behind the ears) being notorious for producing slightly wider scars. Patients with a tendency to form wide scars can produce scars of 5-15 mm in width, but this is very uncommon.
Most linear FUT scars are well concealed by hair worn at least grade 4 in length at the back and sides of the head. If an FUT patient shaves their head in the future the donor scar will be visible. Scar revision procedures, scalp micropigmentation (SMP) and follicular unit excision (FUE) technique grafting into FUT/Strip scars can help to improve their appearance. Choice of hair restoration options
Choice of hair restoration options
Every patient has the choice of various treatment options for their hair loss. These include surgical options such as follicular unit excision (FUE), follicular unit transplantation (FUT)/strip, scalp reduction surgery, flap transfers etc. There are also non-surgical options such as platelet-rich plasma scalp injections, micro needling, low level laser therapy (LLLT), finasteride, minoxidil, vitamin and mineral supplements or doing nothing. Cosmetic options are also available, such as hair systems/wigs, concealer fibres or scalp micropigmentation.
Not infrequently, patients may be advised that surgical and/or non-surgical treatments are not appropriate.
There are potential risks associated with medical or surgical hair restoration. Risks and benefits of both surgery and medication are discussed during our medical consultation. Patients are provided with our surgical consent form during the initial consultation process to assist with informed consent. Patients taking hair loss medication are encouraged to carefully read the patient information leaflets associated with their medication and to discuss any concerns with a doctor or pharmacist.
Removal of stitches following FUT/strip surgery
If undergoing an FUT/strip hair transplant, your stitches will need to be removed 10-12 days after your surgery. We encourage you to return to The Maitland Clinic for your stitch removal. However, if the distance is too far for you to travel you may choose to ask your local GP practice nurse to remove the stitches. It would be wise to contact them well in advance to check that they are happy to remove your stitches.
We suggest you request a 20-30 minute appointment because the wound can be 10-30 cm long with multiple stitches. We will provide a discharge letter containing information regarding your procedure and explaining how we recommend the stitches be removed.
Smoking
Smoking has a negative effect on wound healing and graft survival. The risk of infection and skin necrosis is likely to be higher in smokers. We strongly recommend that smokers see their GP, practice nurse or local NHS quit smoking service to obtain advice and support in advance of surgery. We also have advice on drinking beer and other alcohol after a hair transplant.
Recovery
In your aftercare pack we include Liposomal ATP spray (adenosine triphosphate – an energy provider to healing cells). This encourages rapid healing and improved graft survival. We also provide a soft memory foam neck pillow for use during the first week after surgery, some mild shampoo, ointment for the donor area and painkillers and anti-inflammatory tablets.
Antibiotics are not routinely used after a hair transplant because it is a clean procedure and we must try to reduce the risk of antibiotic resistance. In the event of persisting or increased discomfort, feeling unwell, worsening redness, crusting or discharge from an incision, we encourage prompt contact with a doctor inorder to consider whether antibiotics or a wound swab is required.
As you leave the clinic it is best to leave the grafts exposed, but if you wish to conceal the treated areas it is best to bring a loose, zip-up hooded top. You may wish to bring a selection of hats so that we can advise you on the safest headwear during the recovery period.
We strongly discourage driving home on the day of surgery. We like to offer a mild sedative which cannot be used if driving. We are able to recommend convenient local hotels or taxi services.
Transplanted follicular unit grafts are extremely delicate and must not be touched until the 6th day after your surgery. Your surgical team will teach you how to wash and look after your hair transplant and you are most welcome to attend the clinic for hair washes after your procedure.
It is uncommon for the transplanted hairs to grow straight after surgery. Instead, the transplanted hair shafts will fall out approximately 1-4 weeks after surgery. The stem cells will have healed under the skin and will develop new hairs which start to become apparent after 4-6 months. One week after your hair transplant, it is advisable to wash your hair with some manual pressure to encourage these original transplanted hairs to shed. This prevents any retained, non-growing hair shafts from irritating the skin and causing inflammation or pimples.
We ask you to send us photographs of the recipient and donor areas on day 1 and 10 post-operatively (and any other time that you have concerns or questions). We have a dedicated aftercare phone number for you to call or send WhatsApp photos to. We are available any time to answer questions during your recovery.
Newly transplanted hair generally appears after 4-6 months following surgery. It can take 12-18 months for maximal graft growth to take place.
We will be in touch via email every few months to check on your progress and would like to see you for a post-op review 12 months after your procedure.










